NORD supports comprehensive medical nutrition coverage for any condition where medical nutrition is a medically necessary component of effective treatment for rare disorders.
What is medical nutrition?
Medical nutrition refers to specialized formulas and foods prescribed by a physician to treat specific diseases or conditions with unique nutritional needs. Under the Federal Food, Drug, and Cosmetic Act, medical nutrition is defined as “a food which is formulated to be consumed or administered enterally under the supervision of a physician and which is intended for the specific dietary management of a disease or condition for which distinctive nutritional requirements, based on recognized scientific principles, are established by medical evaluation.”1
Why it matters
For many rare disorders, medical nutrition is the only effective treatment available. Conditions such as maple syrup urine disease, food protein-induced enterocolitis syndrome (FPIES), and short bowel syndrome rely on medical nutrition to prevent serious disability, support normal growth, or provide adequate nutrition. Without insurance coverage, families are often forced to pay significant costs out of pocket.2
What we’re measuring
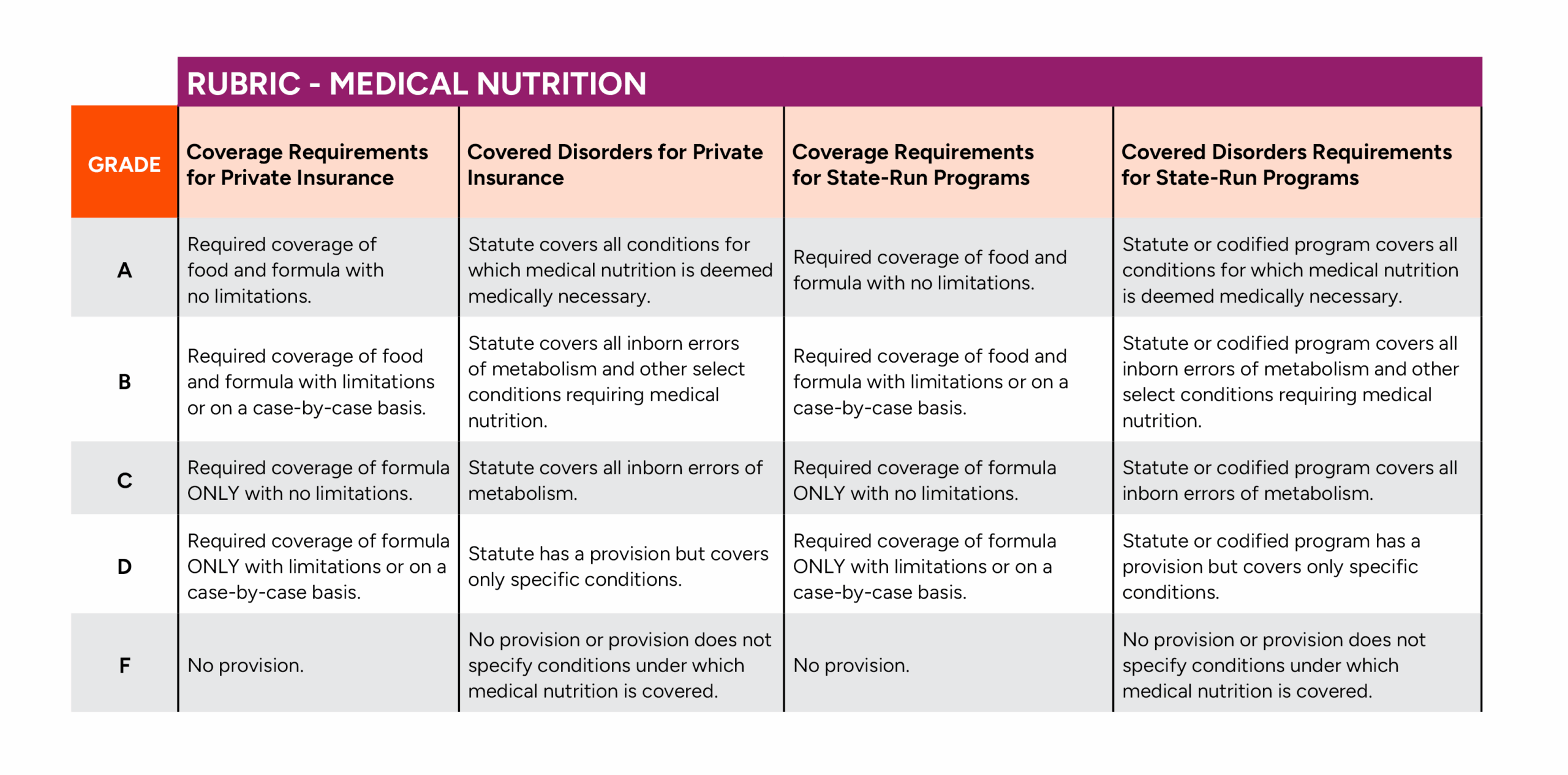
This measure evaluates state Medicaid programs and private insurance requirements for medical nutrition coverage in two key areas:
How we grade
Higher grades are awarded to states with comprehensive coverage mandates that apply broadly across conditions and impose the fewest restrictive coverage requirements.
The coverage problem
Insurance coverage for medical nutrition is inconsistent and varies widely based on a patient’s diagnosis, insurance plan type, and state of residence. Many insurers deny coverage for medical nutrition because the U.S. Food and Drug Administration (FDA) does not regulate it as a drug. In addition, insurers may incorrectly view medical nutrition as a voluntary choice rather than the life-saving treatment it often represents. As a result, many patients who depend on medical nutrition face significant financial barriers to care.
Coverage approaches
Medicaid coverage
Some states require their Medicaid programs to cover medical nutrition. However, many states impose limits based on factors such as cost, age, or gender. Other states provide access through separate public health programs or determine coverage on a case-by-case basis, leading to inconsistent and unreliable access to treatment.
The risk of “uncodified” coverage
In some states, Medicaid programs cover medical nutrition in practice but do not require coverage through state law or regulation. Coverage that is not codified lacks legal protection and can be reduced or eliminated suddenly and without warning, leaving patients unable to access necessary products.
Private insurance coverage
Some states require private insurance plans to cover medical nutrition, but these mandates often apply only to inherited metabolic disorders such as phenylketonuria (PKU). More recently, some states have begun expanding coverage to include additional conditions. In states without coverage requirements, patients are typically responsible for paying out of pocket, which can make life-saving treatment financially unattainable.
1. Federal Food, Drug, and Cosmetic Act. 21 U.S.C. § 360ee. 2015.
2. Kumar Dalei S, Adlakha N. Food Regime for Phenylketonuria: Presenting Complications and Possible Solutions. Journal of Multidisciplinary Healthcare. 2022;15:125–136.
Click to enlarge.
Please complete this form to access the requested resource.
