NORD supports policies to better protect patients by reforming step therapy processes
Step therapy is a process by which insurers (public or private) require patients to take one or more alternative medications before they can access the medicine prescribed by their provider. While this is done by insurers as an attempt to control health care costs, step therapy has been increasingly applied with little regard for a patient’s medical situation or treatment history.
When used inappropriately, step therapy protocols can delay necessary treatment and lead to adverse reactions that ultimately increase rather than lower health care costs. For example, when an individual changes insurance plans they may be required by their new insurer to go off a successful treatment and take a less effective medicine. For rare disease patients, the inappropriate use of step therapy is particularly concerning as it can take years to find a diagnosis and a treatment that works.
As the use of step therapy has increased so has the need for states to ensure these requirements do not interfere with appropriate care for patients. It is important to note that in seeking to reform step therapy protocols, NORD does not advocate for ending the practice of step therapy entirely. Instead, the goal of these reforms is to bolster protections for patients while enabling health plans to achieve cost-saving benefits when appropriate.
More than half of all states have instituted protections around the use of step therapy to help patients obtain the care and treatment they need at the right time. In general, these protections:
Grading Methodology
NORD’s State Report Card grades states separately on the following four separate categories and an overall state grade for step therapy was determined by taking the average of these four separate grades:
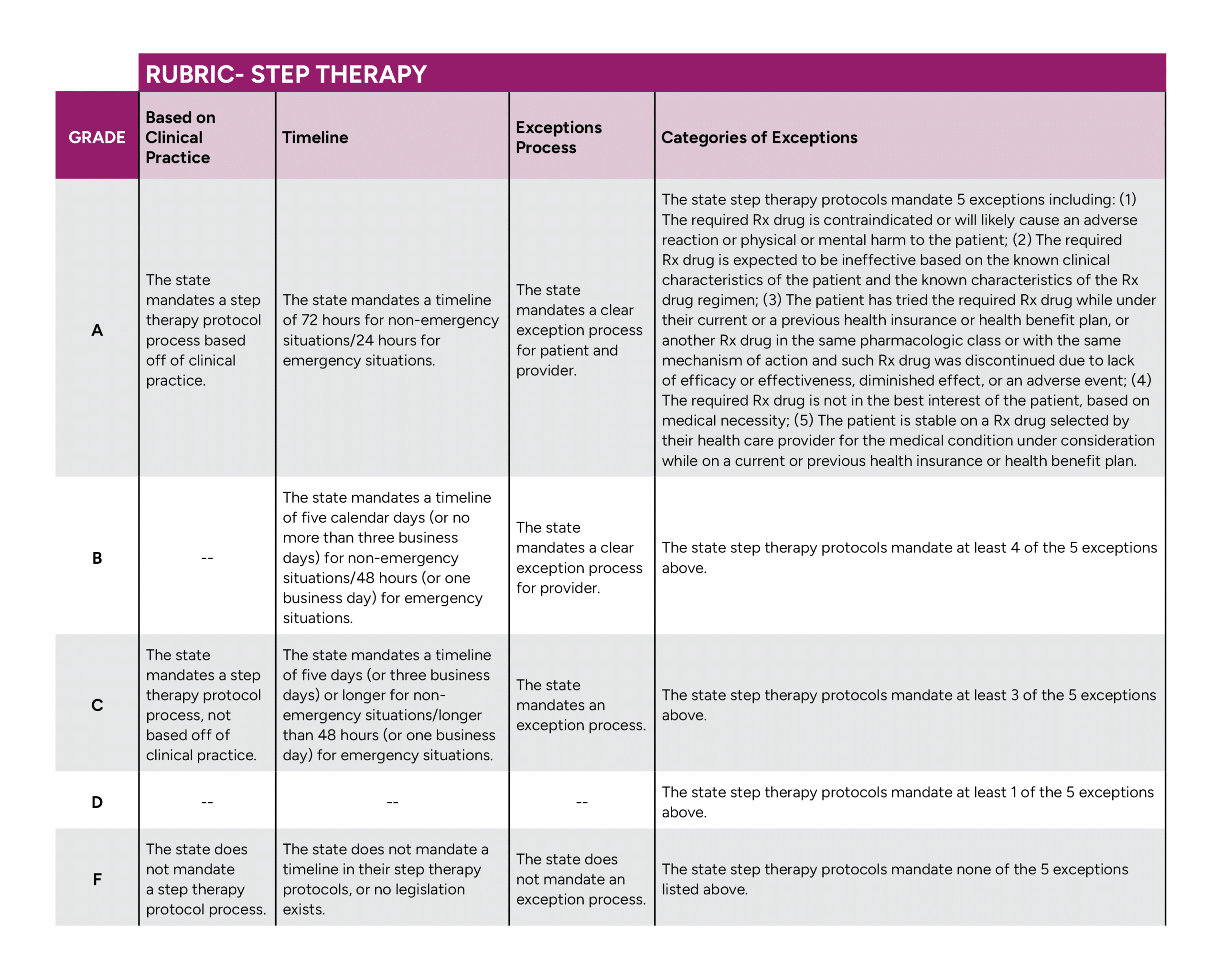
Click to enlarge
